Table of Contents
Ocular surface disease encompasses a range of conditions that affect the outermost layer of the eye, including the tear film, cornea and conjunctiva. These conditions can cause discomfort, vision problems, and even long-term complications if left untreated. As an ophthalmologist practising in Canberra, I believe it is essential to raise awareness and understanding about ocular surface disease among patients.

In this blog, we will explore the causes, symptoms, and treatment options for ocular surface disease.
What is Ocular Surface Disease?
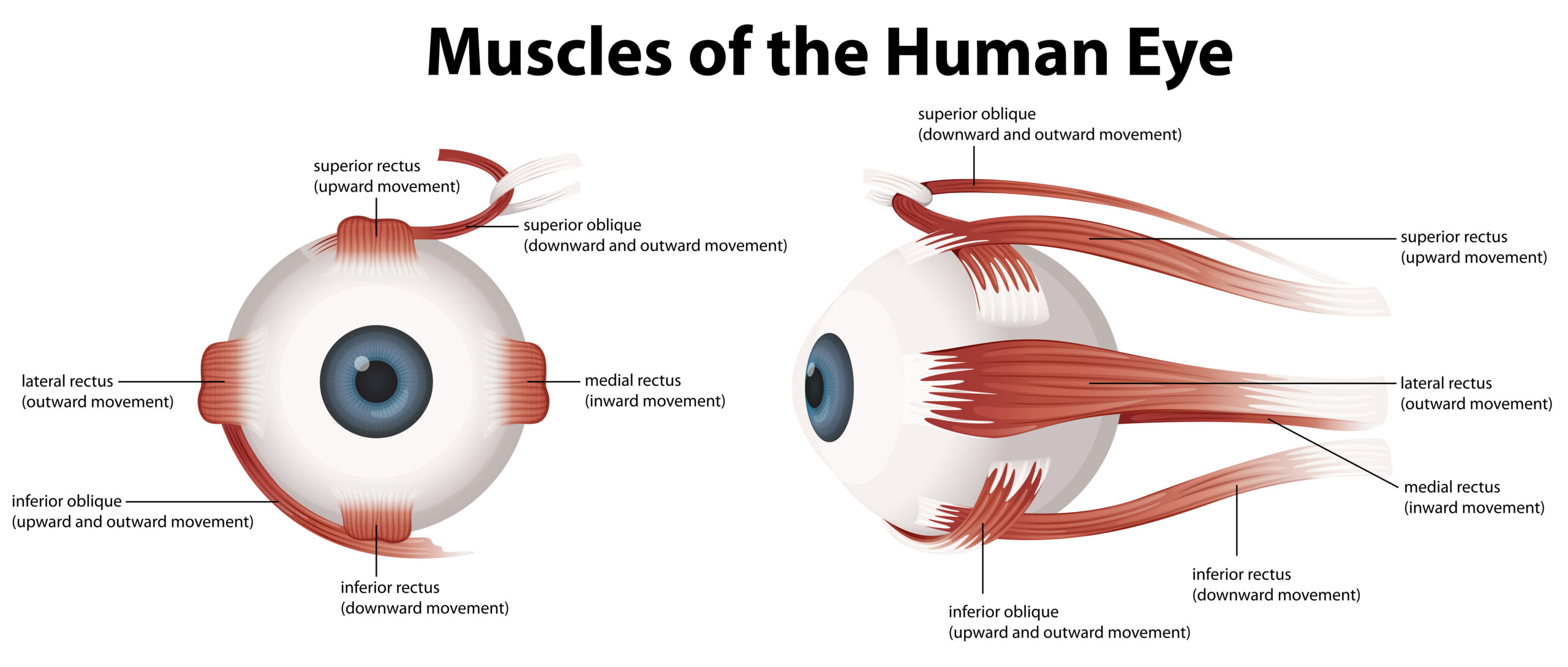
The ocular surface refers to the front part of the eye, which includes the tear film, the cornea (clear dome-shaped window) and the conjunctiva (thin, clear membrane covering the white part of the eye). Ocular surface disease is a broad term that encompasses various conditions affecting these structures. The healthy ocular surface is crucial for maintaining clear vision, as it provides a smooth, clear surface for light to refract through.
Causes of Ocular Surface Disease
- Dry Eye Syndrome: Insufficient tear production and/or poor tear quality.
- Blepharitis: Inflammation of the eyelids, either anterior (outside edge) or posterior (inner edge).
- Allergic Conjunctivitis: An allergic reaction causing conjunctival inflammation.
- Meibomian Gland Dysfunction: Dysfunction or blockage of the glands that produce the oily component of tears.
- Corneal Infections or Injuries: Infections or damage to the cornea, often due to bacterial, viral, or fungal causes.
Certain risk factors increase the likelihood of developing ocular surface disease, such as ageing, hormonal changes, contact lens wear, prolonged digital device use, and environmental factors including dry climate or exposure to smoke.
If left untreated, ocular surface disease can lead to complications such as corneal ulcers, corneal abrasions, and even vision loss in severe cases.
Symptoms of Ocular Surface Disease
- Dryness and a gritty or sandy sensation in the eyes.
- Redness, itching, or burning.
- Excessive tearing.
- Blurred or fluctuating vision.
- Sensitivity to light.
- Feeling of having something in the eye (foreign body sensation).
Diagnosis of Ocular Surface Disease
To diagnose ocular surface disease, your ophthalmologist will perform a comprehensive eye examination, including assessing your tear film quality, checking for corneal staining, and evaluating the health of your eyelids and conjunctiva. Specialised tests may also be used to determine the severity and underlying causes of the disease.
Treatment Options:
The treatment approach for ocular surface disease depends on the underlying cause and severity. Some common treatment options include:
- Artificial Tears and Lubricating Eye Drops: These over-the-counter or prescription eye drops help alleviate dryness
- Prescription Medications: Depending on the specific condition, your ophthalmologist may prescribe anti-inflammatory medications, immunosuppressive drugs, or antibiotics to address underlying inflammation, infection, or gland dysfunction.
- Eyelid Hygiene and Warm Compresses: Regular eyelid hygiene, including gentle cleaning and warm compresses, can help manage blepharitis and improve tear quality.
- Punctal Plugs: These tiny devices are inserted into the tear ducts to block the drainage of tears, thereby increasing tear retention and lubrication of the ocular surface.
- Lipid-Based Therapies: Lipid emulsion eye drops or oral supplements containing omega-3 fatty acids may be recommended to improve the quality of the oily component of tears.
- Surgical Interventions: In severe cases or when other treatments fail, surgical options such as punctal occlusion and meibomian gland expression or probing may be considered.

It is important to remember that treatment plans should be tailored to each individual’s needs, and regular follow-ups with your ophthalmologist are crucial to monitor progress and adjust the treatment as needed.
Lifestyle Modifications and Prevention:
In addition to medical interventions, making certain lifestyle modifications can help manage ocular surface disease and prevent its worsening. Consider the following tips:
- Environmental Modifications: Use a humidifier in dry indoor environments, avoid exposure to smoke, and protect your eyes from harsh winds and dusty environments.
- Proper Eye Hygiene: Clean your eyelids and lashes regularly, especially if you have blepharitis, using a gentle cleanser recommended by your ophthalmologist.
- Nutrition and Hydration: Stay well-hydrated, as dehydration can exacerbate dry eye symptoms. Include foods rich in omega-3 fatty acids, such as fish, flaxseed, and walnuts, in your diet.
- Regular Eye Examinations: Schedule regular eye exams with your ophthalmologist or optometrist to detect ocular surface disease early and receive appropriate treatment.
Managing Ocular Surface Disease in Specific Populations:
Certain populations may be more susceptible to ocular surface disease or require additional considerations:
- Older Adults: Aging can contribute to decreased tear production and changes in tear quality. Regular eye exams and appropriate treatment can help manage ocular surface disease in older adults.
- Contact Lens Wearers: Proper contact lens hygiene, including cleaning and disinfection, is crucial to prevent ocular surface infections and irritation. Consult with your eye care professional for specific recommendations.
- Computer or Digital Device Users: Prolonged digital device use can lead to dry eye symptoms.

Collaborating with Ophthalmologists:
To ensure accurate diagnosis, effective treatment, and personalised care, it is essential to collaborate with ophthalmologists who specialise in ocular surface disease. Regular follow-ups, open communication, and adherence to treatment plans are vital for managing and improving the ocular surface health.
Conclusion:
Ocular surface disease can significantly impact your eye health and quality of life. By understanding the causes, recognising the symptoms, and exploring the available treatment options, you can take proactive steps to manage ocular surface disease effectively. Remember, early detection, professional guidance, and consistent self-care practices are key to maintaining optimal ocular surface health. Schedule regular eye exams, communicateopenly with your ophthalmologist, and prioritise your eye health to enjoy clear vision and ocular comfort for years to come.